Awake fiberoptic orotracheal intubation using a modified Guedel airway in a patient with craniocervical instability and an anticipated difficult airway - A case report -
Article information
Abstract
In patients with upper cervical instability, airway management may provoke subluxation of the craniocervical region and neurologic injury, and can be challenging for the anesthesiologist. Endotracheal intubation using a fiberoptic bronchoscope is frequently used in these patients to minimize spine motion, but this procedure may fail in patients with altered airway anatomy. When fiberoptic endotracheal intubation fails in these patients, optional intubation methods are limited. We describe successful awake fiberoptic orotracheal intubation using a modified Guedel airway divided in the midline for a 59-year-old man with an anticipated difficult airway, due to limited mouth opening, a nasopharyngeal tumor, and craniocervical spine instability after failure of conventional fiberoptic orotracheal intubation.
The guidelines for airway management in patients with craniocervical spine instability remain unclear. Mask ventilation and endotracheal intubation in these patients with Philadelphia collars is considered difficult. Nevertheless, movement of the cervical spine during tracheal intubation must be avoided because of the risk of neurologic injury from compression of the spinal cord and brain stem [1]. Various procedures and devices are used to assist tracheal intubation in patients with an unstable cervical spine. These include a lightwand, videolaryngoscopic devices, retrograde intubation, the laryngeal mask airway, fiberoptic bronchoscope (FOB)-guided intubation, and the malleable fiberoptic stylet. Among these, awake fiberoptic nasal or oral endotracheal intubation (FOI) have been preferred to minimize spine motion in both surgeons and anesthesiologists. However, conventional FOI may fail in these patients because of difficulty in advancing the fiberoptic bronchoscope into the trachea. In contrast with the nasal route, a higher failure rate was reported with the oral approach and may be due to the difficulty of positioning the scope in the midline [2].
Various oral airways are commercially available to overcome this problem during FOI. In a study of these airways, all had various problems with functionality and were frequently unable to allow a clear passage for the FOB without a skilled assistant and extra assistance such as head tilt with chin lift, jaw thrust, and teeth protruding [3]. Moreover, few institutions are equipped with all commercially available airways or various devices for airway management. We previously experienced a patient with an unstable craniocervical spine who finally underwent tracheostomy, because of failure on several attempts to insert an FOB into glottis. However, we could easily find an edematous glottis through an FOB introduced into a conventional Guedel oral airway. Therefore, a conventional Guedel airway was modified into a shape divided to assist with difficult FOI and advancement of an endotracheal tube. We experienced a patient with anticipated difficult airway due to limited mouth opening, nasopharyngeal tumor, and an unstable craniocervical junction, and report successful awake FOB insertion using this modified Guedel airway.
CASE REPORT
A 59-year-old male (body weight 55 kg, height 169 cm) with American Society of Anesthesiologists physical status classification 2 was scheduled for occipitocervical fusion. He had nasopharyngeal cancer and underwent radiotherapy, cyber knife treatment, and chemotherapy in 2007. He had a relapse after 10 years, and received radiation therapy for 5 months. After radiotherapy, he developed trismus, hypothyroidism, and neck pain and stiffness. Magnetic resonance imaging revealed radiation necrosis at the C1-2 level and skull base, C1-2 instability, mild narrowing of the central canal at the C1 level, recurrent nasopharyngeal cancer, and radionecrosis of the nasopharynx (Fig. 1). On physical examination, his interdental distance was about 1.5 cm, and his neck was very rigid and stiff because of fibrosis and induration of surrounding and overlying neck tissue. Thyromental distance and Mallampati class were not measured due to insufficient mouth opening and the use of a Philadelphia collar. The surgical staff requested awake intubation during the induction of anesthesia. Therefore, we planned awake FOI with the Philadelphia collar around his neck. The patient was informed about the procedure and was reassured. He was premedicated with glycopyrrolate 0.2 mg intramuscularly. After arrival in the operating room, standard monitors (electrocardiogram, capnography, pulse oximetry, noninvasive blood pressure) were applied. For topical anesthesia, 10% lidocaine was sprayed on the tongue and oropharynx, and cricothyroid injection of 3 ml of 2% lidocaine was performed. Thereafter, the patient was administered oxygen (4 L/min) via nasal cannula and received propofol and remifentanil at an effect-site concentration of 1–2 μg/ml and 0.5–1.5 ng/ml, respectively, for procedural sedation. A fiberoptic bronchoscope (3.5 mm diameter, Pentax Fi-10RBS, Hoya Co., Japan) was inserted into a lubricated reinforced tube (7.0 mm inner diameter, Mallinckrodt, USA). An FOB was introduced orally but failed to locate the glottis on repeated attempts over 20 minutes. We decided to use modified Guedel airway prepared previously for difficult awake FOI. While modifying the airway, we asked the cutting procedure of the airway of a medical equipment management team, that easily cut the airway longitudinally along the midline from the proximal flange to the distal tip by using electric drill rotatory tool with cutting piece, and scraped down the edges of the divided airway. We applied silicone tape (Inomed, Ahejang Longterm Medical Technology Co., Ltd, China) with more regular slits at the midline than original tape by making a few silts; the tape was easily divided with light traction, and was only used to cover the lingual concave aspect because adequate fixation of the divided airway could be obtained (Fig. 2). The modified airway could be divided after separation at the slits of tape by light pressure and provide a room for the insertion of endotracheal tube after the removal of one side of separated airways and prevent from bite of patient through another side of airway remained in the oral cavity.
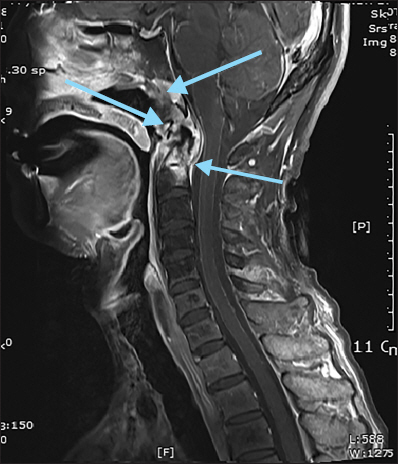
Magnetic resonance imaging of the patient’s cervical spine, demonstrating skull base and C1 and C2 radiation necrosis with C1-2 instability, recurrent cancer in the nasopharynx, and narrowing of the central canal at C1 level.

Modified Guedel airway cut in midline and fixed with silicone tape; the tape had more regular slits at the midline than original tape by making a few slits (A) and was easily divided by light traction (B).
We inserted the sterilized modified Guedel airway into the oral cavity and then advanced the FOB threaded into the endotracheal tube along the airway. We immediately located the glottis area after inserting the FOB. When the glottis was visualized, the FOB was advanced through the vocal cords until the carina was visualized. The endotracheal tube was then advanced to the correct position after dividing the airway by light traction and removing one part of the divided airway. The entire process starting from insertion of the modified Guedel airway to successful tracheal intubation required less than 5 minutes. Oxygen saturation remained above 96% throughout the entire process. Total intravenous anesthesia was induced using propofol, remifentanil, and rocuronium. The invasive monitors were applied, and the patient was moved to the prone position. Thereafter, occipitocervical fusion was performed under standard general anesthesia for 6 hours. After the surgery, the patient was extubated uneventfully while awake. The postoperative period and the recovery were also uncomplicated.
DISCUSSION
Anticipating a difficult airway is critical for an optimal anesthetic management, because repeated unsuccessful attempts at endotracheal intubation may cause airway edema, injury, and bleeding, leading to a “cannot ventilate, cannot intubate” situation. Additionally, airway management in a patient with an unstable upper cervical spine is a challenge, requiring prevention of neck motion, for anesthesiologists. We demonstrate a patient with an anticipated difficult airway and an unstable craniocervical spine who underwent uneventful airway management using a modified Guedel airway for FOI.
Conventional FOI may occasionally fail in patents without a difficult airway, and more frequently fails when a difficult airway is anticipated. Failure rates of 4–66% for fiberoptic tracheal intubation have been reported [4]. Endotracheal intubation using an FOB may be performed more easily by the nasal route than using an oral approach because the bronchoscope tip can be maintained stably in the midline of the airway and in a straight position to access the vocal cord [2]. However, in our patient, nasal FOI was not possible because of the risk of injury and bleeding from the nasopharyngeal tumor. FOI may be very time-consuming because of the lack of a guided trajectory for the bronchoscope, and requires a skilled anesthesiologist in cases with difficult airways. Various commercially available oral airways have been developed for overcoming these difficulties during FOI. Each airway has a channel that allows for passage of the FOB [3]. The Patil-Syracuse airway and the Williams airway intubator have anterior channels, but the Ovassapian airway and Luomanen airway have posterior channels. The anterior channel of the Patil-Syracuse airway is too small to allow passage of an endotracheal tube, and must first be removed. In contrast, the Williams airway permits endotracheal tube passage through the anterior channel after detaching the circuit adaptor. However, this device cannot easily be removed, and even then may result in loss of tube position. Moreover, damage to the tracheal cuff is not uncommon if a large and less lubricated endotracheal tube is used. A modified Williams airway intubator may cause tongue or lingual tonsillar material to herniate into the airway. The Ovassapian airway has been known to cause damage to the cuff of the endotracheal tube. One study comparing commercially available airways found that all had major problems with functionality [3]. A 43% FOB insertion failure rate was found with the Ovassapian airway. Oral airways with a posterior channel, such as the Ovassapian airway, may limit access to a glottis that is located laterally and off midline. In fact, few operating rooms are equipped with various commercially available oral airways. Our modified Guedel airway can be prepared easily and immediately in most operating rooms when a difficult airway is anticipated and awake FOI is required. Additionally, it may provide lesser difficulties from the removal of airway after successful endotracheal intubation and lesser damages of the cuff of the endotracheal tube than other modified airways.
Adequate airway support with lingual traction, the jaw-thrust maneuver, head tilt with chin lift, and teeth protruding may be effective for FOB insertion, but these cannot be used in patients with an unstable cervical spine [5]. Upper cervical spine movement during endotracheal intubation in patients with instability may cause neurologic injury. Intubation using direct laryngoscopy and other devices, such as the Bullard laryngoscope, intubating laryngeal mask airway, lightwand, and Glideoscope, have been known to produce varying degrees of extension at the occipitocervical junction [1,6,7]. Postoperative neurologic injuries that seemed to be associated with intubation using direct laryngoscopy have been reported in patients with an unstable occipitocervical junction or cervical spine trauma [8].
The most appropriate technique for achieving successful endotracheal intubation in a patient with cervical spine instability is unknown. Some studies have assessed cervical spine motion with use of various airway devices or procedures. The elevation of laryngeal structures with a direct laryngoscope can cause extension of the C1-2 joint, whereas the C3-5 joint is minimally displaced [9]. Brimacombe et al. [10] found significant movement of the destabilized cervical spine during face mask use, orotracheal intubation using direct laryngoscopy, esophageal tracheal Combitube use, laryngeal mask insertion with fiberoptic-guided tracheal intubation, and laryngeal mask airway use, but not with fiberoptic nasal intubation. Awake FOB-guided tracheal intubation has been preferred among surgeons and anesthesiologists in these patients. Most surgeons also want their patients anesthetized when applying a Philadelphia Collar or spinal traction. A Philadelphia collar limits mouth opening, restricts neck movement, and makes the airway management procedure including mask ventilation, laryngoscopy, and endotracheal intubation difficult. An intubating laryngeal mask airway may provide an adequate alternative for awake FOI with cervical immobilization with halo traction [11]. However, we could not attempt insertion of a laryngeal mask airway because the mouth opening was not adequate for insertion of this device. Furthermore, because of its size, the laryngeal mask airway can potentially cause airway trauma and bleeding, which can interfere with FOI. The limitations of a laryngeal mask airway may also apply to endotracheal intubation when an airway tumor is present or the glottis is off midline. We also considered endotracheal intubation using a lightwand, which can be used in patients with trismus, and which induces less cervical movement than other devices including the Airtaq laryngoscope, intubating laryngeal mask airway, and Macintosh laryngoscope [12]. However, general anesthesia is usually required during intubation with the lightwand because the procedure may be uncomfortable under conscious sedation. General anesthesia causes the soft palate, tongue, and epiglottis to be displaced backwards to the posterior pharyngeal space and hypopharynx, and hinders passage of FOI. In patients with a difficult airway, general anesthesia may lead to a catastrophic “cannot mask ventilate, cannot intubate” situation. Therefore, we did not try to intubate using a lightwand under general anesthesia.
A limitation of our modified Guedel airway is that it cannot be threaded by a large-size FOB or inserted into the oral cavity in patients with severe trismus. The larger gap between a fiberscope and a tracheal tube may easily cause impingement of surrounding tissue, such as arytenoids or epiglottis, and cause more difficulty in advancing the endotracheal tube [13]. This problem can be overcome by use of a tapered tube, a gap-filler, or warming and rotation of the tube. Some reports have described a modified conventional Guedel airway [14,15]. These airways had large channels for passage of a large fiberscope, but were too small to permit the passage of a tracheal tube, and must be removed first before advancing a tube. A sedated patient may bite an FOB or endotracheal tube after removing the airway. We left half of a modified Guedel airway in the oral cavity of a patient to protect against the injury of a bronchoscope or difficulty in advancing the endotracheal tube due to biting by the patient. It is necessary to verify the usefulness of the modified Guedel airway for FOI in a larger number of patients with unstable cervical spines. In this case, we did not examine motion of the cervical spine but the entire procedure was performed with the neck collar in place. Moreover, the patient recovered without a neurologic deficit during the postoperative period.
In conclusion, we report use of a modified Guedel airway that was divided in the midline to enable awake FOI in a patient with an unstable craniocervical spine, difficult airway, and unavailable nasal intubation during cervical immobilization with a Philadelphia collar.