INTRODUCTION
The beach chair position is often used for anatomical orientation and visualization of the surgical site in orthopedic shoulder surgery. However, beach chair positioning has the reported risk of iatrogenic nerve damage, specifically involving the supraclavicular, axillary, musculocutaneous, subscapular and spinal accessory nerves following arthroscopic surgery [
1,
2].
Cases of greater auricular nerve (GAN) injury following shoulder arthroscopic surgery are reported sporadically [
3-
5]; however, there are no reports of GAN injury following fracture of the clavicle. The GAN runs obliquely across the sternocleidomastoid muscle along its posterior border dividing into an anterior and posterior branch. It arises in C2 and C3 spinal nerves and innervates the skin covering the mastoid process and parotid gland [
6,
7]. Compression nerve injury from usage of a horse-shoe headrest or a standard universal headrest was the cause of GAN injury in three cases reported previously. However, greater auricular nerve neuropraxia (GANN) has not been previously reported in beach chair positioning using intubation pad-type headrest (
Fig. 1).
Fig. 1
Neck position of the patient during the surgery, as reproduced by the model.

Herein, we reported a case of GANN following beach chair positioning using an intubation pad-type headrest with review of the relevant literature.
CASE REPORT
A 49-year-old Asian man was diagnosed with left clavicular fracture due to a fall from a bicycle. The patient had no surgical or medical history; and there was no accompanying injury or complication. The patient was scheduled for open reduction and internal fixation with a plate.
The surgery was performed under general anesthesia. In the operating room, the patient was monitored for electrocardiography, pulse oximetry, non-invasive blood pressure, and bispectral index. Anesthesia induction was with fentanyl 100 μg, propofol 120 mg, and rocuronium 50 mg. After muscle relaxation, the patient was intubated with an 8 mm-cuffed oral endotracheal tube. Anesthesia was maintained with 1 L/min oxygen, 2 L/min air, 2 vol% sevoflurane; the ventilator setting was tidal volume 500 ml and respiratory rates of 12/min; and the bispectral index was maintained within 40-60. Sixty min after the start of anesthesia, rocuronium 10 mg was administered to increase muscle relaxation. The patient was maintained in standard beach-chair-position using a beach chair (T-MAX Shoulder Positioner®, Smith & Nephew, USA), at 45° upright from the operation room floor with hip flexion 60° and knee flexion 30°. A pneumatic compression device was used for the lower extremities, the body trunk was secured with lateral support knobs, and the head was fixed with an intubation pad-type headrest in the neutral position. Just before surgery, the patient’s neck was adjusted to right deviation 20° extension 10°, right rotation 5°, and atlanto- occipital joint extension 10°. The surgery was conducted in consistent position for 110 min in total. Emergence from anesthesia was as follows. The patient was moved from the beach chair onto a stretcher car turned to supine position; after intravenous injection of sugammadex 200 mg and regaining self-respiration, the patient underwent extubation. The patient was observed in a recovery room for an additional 60 min and then transferred to a ward. Post-surgical pain was treated with intravenous patient-controlled analgesia. The remainder of the postoperative course was uneventful.
The same night, the patient reported numbness and a tingling sensation in the auricular area and the lower margin of left mandible; however, there was no pain or skin lesion in the corresponding area. GANN was diagnosed based on the results of otolaryngology and neurology consultation. Outpatient department follow-up was scheduled to accompany procedural observation.
At the two weeks outpatient follow-up, the patient’s numbness and tingling sensation was decreased by 50%; and in the following two weeks, the patient reported complete disappearance of the symptoms.
DISCUSSION
We reported a rare case of GANN after open reduction and internal fixation with plate of clavicular fracture in beach chair positioning, despite using an intubation pad-type headrest. Shoulder surgery is commonly conducted with the patient in beach chair position. Beach chair position results in decreased traction injury of the brachial plexus in arthroscopic surgery, as compared to lateral decubitus position [
8]; hence, it is used in cases of clavicular fracture surgery by open reduction and internal fixation with plate, for easy exposure and access to the operation site.
However, inappropriate head and neck positioning can cause neurologic complications; and thus, a headrest has been used in conjunction to avoid unwanted changes in position of the head and neck. The commonly used horse-shoe headrest consists of a thickened horse-shoe-shaped cushioned boundary that meets the patient’s head. Also, a circumferential strap is attached to the headrest to secure the head in position. Park and Kim [
3] reported neural compression leading to GANN from use of the horse-shoe headrest; and suggested the need to adjust the headrest design according to patient’s physical figure and occiput size. Ng and Page [
5] also reported that the horse-shoe headrest pillow compresses the branches of GAN and causes related neuropathy. Therefore, universal standard headrests have been introduced to prevent risks from using a horse-shoe headrest. However, LaPrade and Foad [
4] reported cases of GANN even when a horse-shoe headrest was replaced with a universal standard headrest. Herein, we reported a case of GANN following use of an intubation pad-type headrest. This is the first case of GANN from use of an intubation pad-type headrest in a beach chair position for open reduction and internal fixation of clavicular fracture.
The intubation pad-type headrest comprises soft foam and lacks structure that would pressure the nerves directly. Therefore, it is difficult to explain the cause of nerve neuropraxia by headrest compression. Two alternative possibilities include the patient positioning that itself caused stretching injury of GAN, or compressive injury due to excess extension of skin, subcutaneous tissue, and sternocleidomastoid muscle. We studied the changes of patient’s nerve diameter in the GAN, using ultrasound images, based on the changes in position of the neck between the neutral position and the surgical position: right deviation 20°, extension 10°, right rotation 5°, and atlanto-occipital joint extension 10°. The results showed that the GAN diameter was larger in the neutral position than in the surgical position (
Fig. 2). Therefore, we more specifically evaluated the effect of each position factor in the surgical position on nerve diameter. Unlike the other factors, the nerve diameter showed a decrease at 5° neck rotation. In addition, as the rotation increased, the diameter decreased further (
Fig. 3). Neck rotation that maximally stretches the nerve in parallel with the direction of the greater auricular nerve is likely to have caused tension in the surrounding tissue due to SCM muscle contraction, thus reducing the diameter of the GAN. Similar effects have been shown in a study on the median nerve activity at different wrist positions [
9]. Other than patient position, the determinants of GANN also include the duration of operation or the possibility of GAN variation [
4,
10]. However, 110 min is not considered a prolonged duration for a shoulder operation conducted in the same beach chair position. Moreover, the patient’s symptom follows the typical sensory distribution of GAN, eliminating the possibility of nerve variation.
Fig. 2
Reduction in the diameter of the greater auricular nerve due to neck position change. Ultrasound images showing the diameters of nerve in (A) neutral neck position and (B) operative neck position. The arrows indicate the greater auricular nerve.
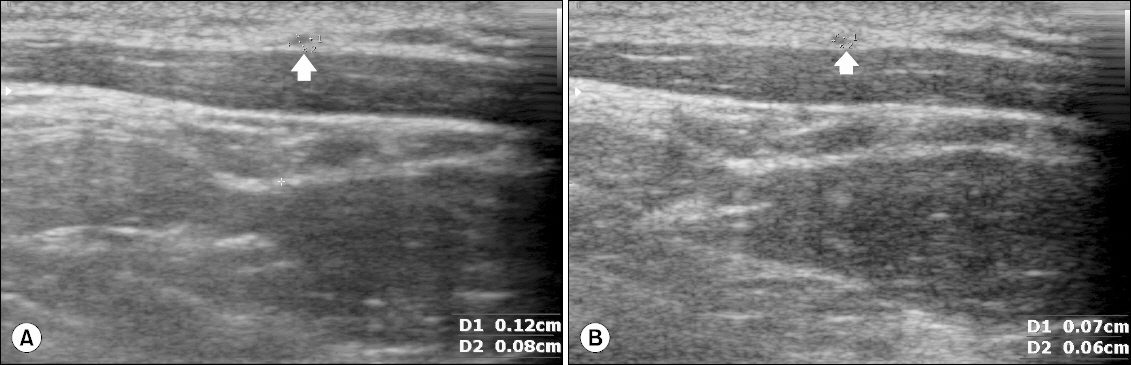
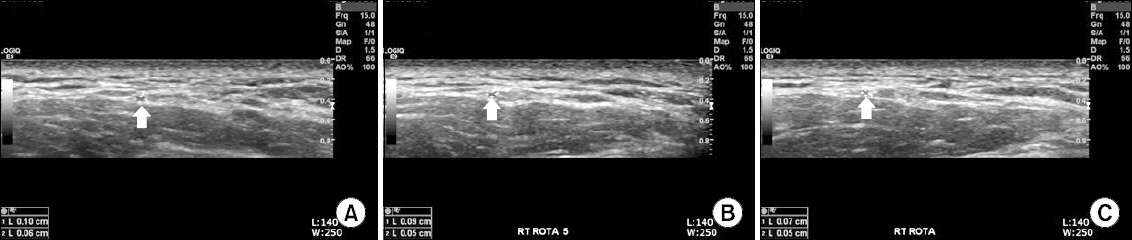
Fig. 3
Decreased greater auricular nerve diameter according to neck rotation; neutral position (A), rotation 5o (B), and full rotation (C). The arrows indicate the greater auricular nerve.
This case report highlighted the possibility of GANN from use of intubation pad-type headrest in a beach chair position. Direct compression of GAN by headrest was ruled out as the immediate cause; however, the neck position that results in nerve stretching damage or compressive nerve injury by perineural structure including the sternocleidomastoid muscle, levator scapulae muscle, and subcutaneous tissue with skin could have a causative effect.






