 |
 |
- Search
| Anesth Pain Med > Volume 18(4); 2023 > Article |
|
Abstract
Background
Methods
Results
SUPPLEMENTARY MATERIALS
Supplementary Table 1.
Supplementary Table 2.
Supplementary Table 3.
Supplementary Table 4.
Notes
DATA AVAILABILITY STATEMENT
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
AUTHOR CONTRIBUTIONS
Writing - original draft: Ji Hyun Park. Writing - review & editing: Seong-Soo Choi. Conceptualization: Seong-Soo Choi, Ji Hyun Park, Seong-Sik Cho. Data curation: Ji Hyun Park, Jongeun Jung. Formal analysis: Ji Hyun Park, Jongeun Jung. Methodology: Seong-Soo Choi. Project administration: Seong-Sik Cho. Visualization: Ji Hyun Park, Jongeun Jung. Investigation:Ji Hyun Park, Seong-Sik Cho. Resources: Seong-Sik Cho, Jongeun Jung.
Software: Seong-Sik Cho, Jongeun Jung. Supervision: Seong-Soo Choi. Validation: Seong-Soo Choi, Seong-Sik Cho.
Fig. 1.
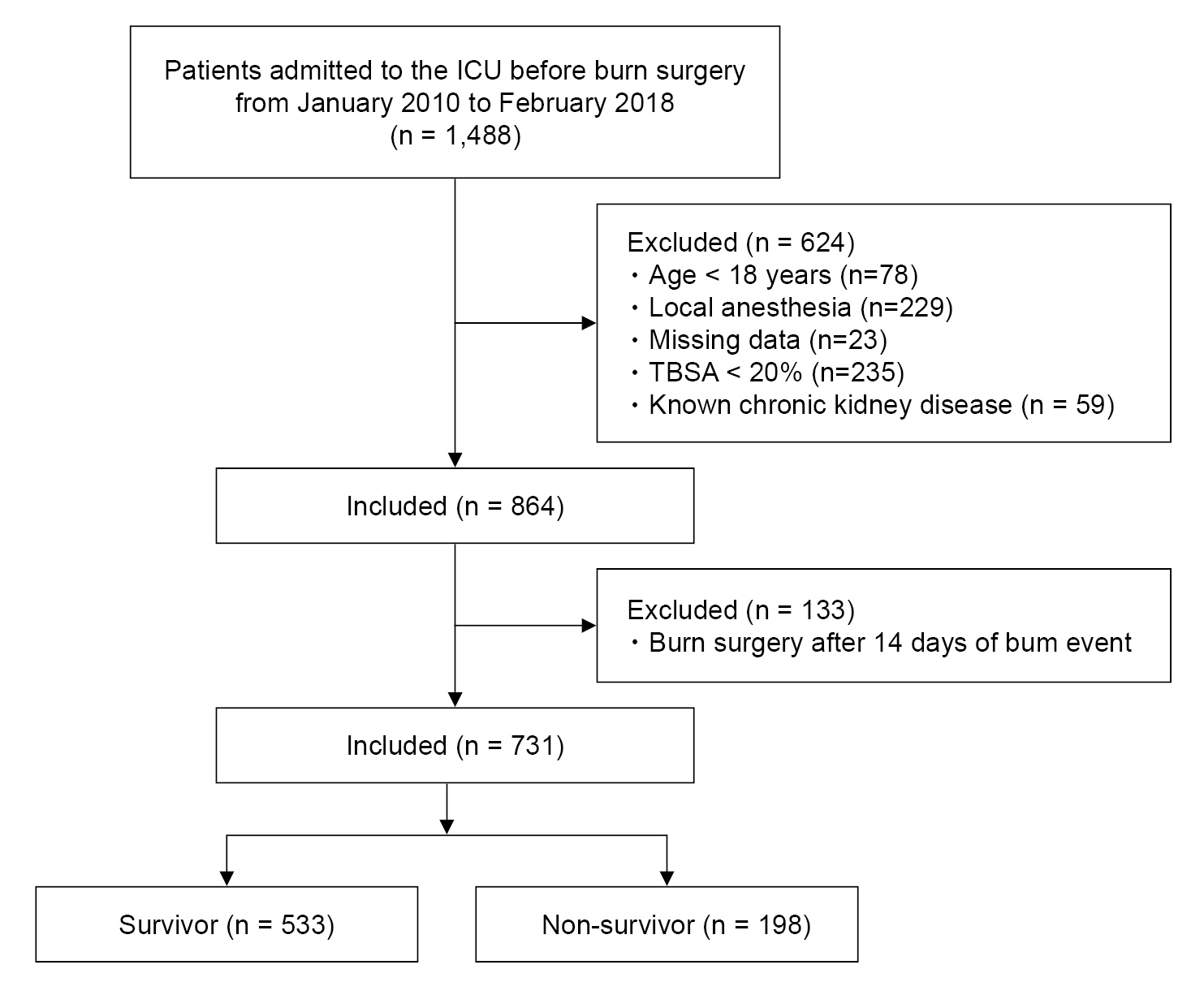
Fig. 2.
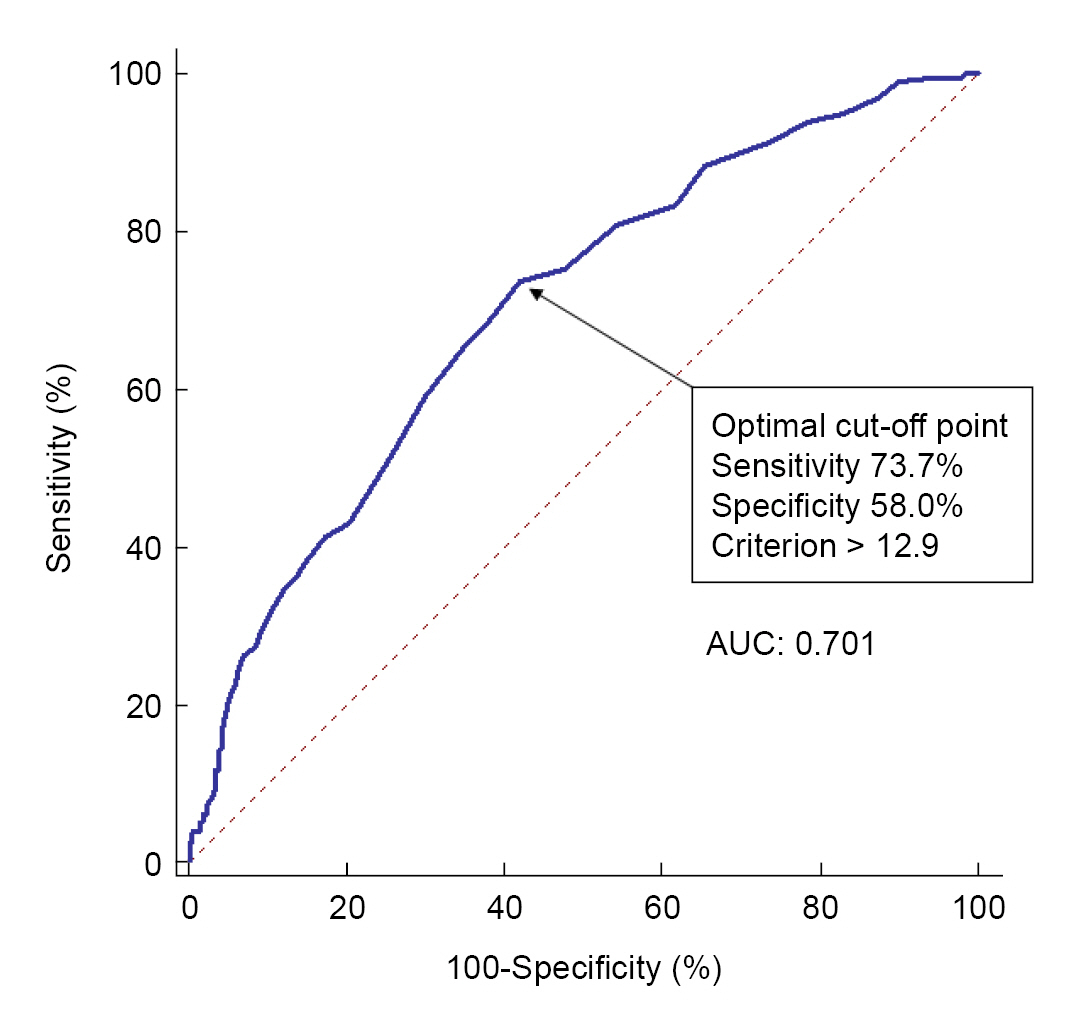
Fig. 3.
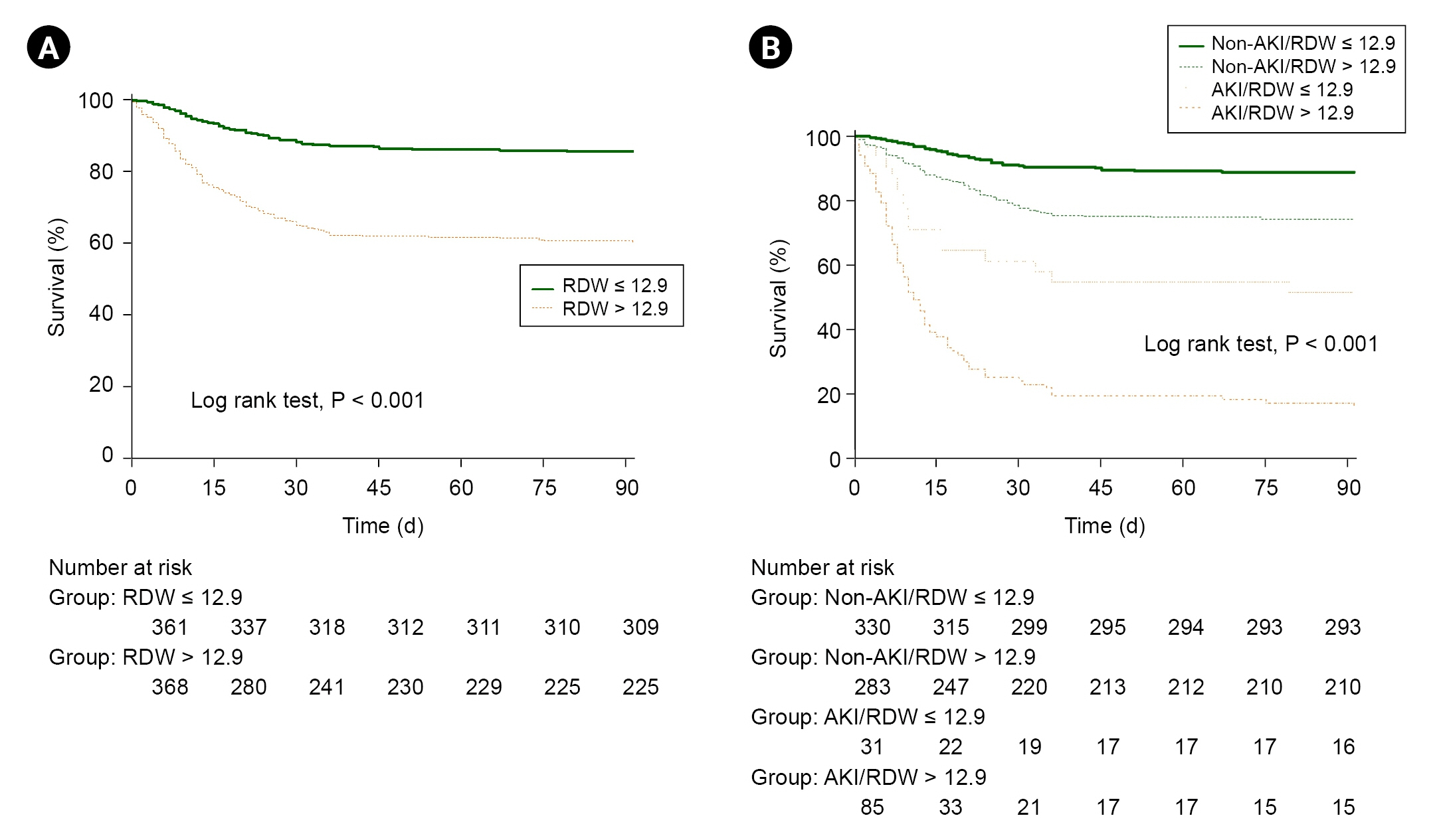
Table 1.
Values are presented as mean ± SD or number (%). RDW: red cell distribution width, ASA PS: American Society of Anesthesiologists physical status, TBSA: total body surface area, Hb: hemoglobin, INR: international normalized ratio, Cr: creatinine, NLR: neutrophil-lymphocyte ratio, PLR: platelet-lymphocyte ratio, MLR: monocyte-lymphocyte ratio, SII: systemic immune-inflammation index.
Table 2.
| Variable | Group |
Crude |
Multivariate adjusted* |
||
|---|---|---|---|---|---|
| HR (95% CI) | P value | HR (95% CI) | P value | ||
| 3-month mortality | RDW ≤ 12.9 (n = 361) | 1 (reference) | 1 (reference) | ||
| RDW > 12.9 (n = 370) | 1.327 (1.239-1.422) | < 0.001 | 1.238 (1.138-1.347) | < 0.001 | |
Table 3.
REFERENCES
- ARTICLE & TOPICS
-
- Topics
-
- Neuroscience in anesthesiology and critical care
- Anesthetic Pharmacology
- Obstetric Anesthesia
- Pediatric Anesthesia
- Cardiothoracic and Vascular Anesthesia
- Transplantation Anesthesia
- Spinal Pain
- Regional Anesthesia
- Neuromuscular Physiology and Pharmacology
- Airway Management
- Geriatric anesthesia and Pain
- Others








